Spinal Stenosis
Appointment Inquiries
Call us at: (877) 222-5348
Definition
The narrowing of the spinal canal which causes pressure to be put on the nervese within the spine
Root Causes
Ankylosing Spondylitis, Arthritis + Osteoarthritis, Bulging + Herniated Discs, Degenerative Disc Disease, Spinal Injury, Tumors
Risk Factors
Age, Birth Defects, Family History, Genetics, Paget's Disease
Treatments
Chiropractic, Diagnostic X-Ray, Massage Therapy, Nutritional Advice, Physical Therapy
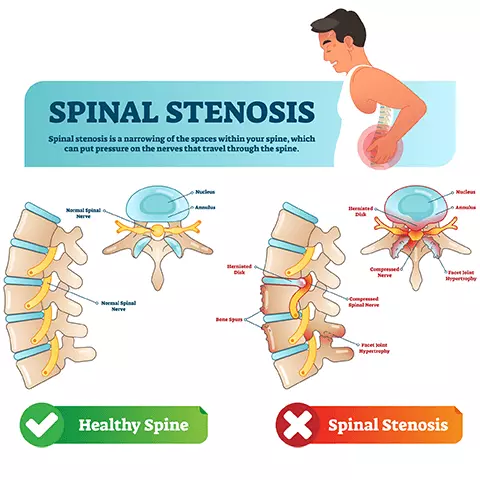
What is spinal stenosis?
The spine is a column of bones called vertebrae that provide support and stability to the upper body. Between every vertebra is soft tissue called the intervertebral discs. These discs act as shock absorbers for your back so you can flex, bend, and twist.
Each vertebra has a hole down its center, as well as holes out each side for the nerve roots. Since they stack on top of each other, together they form a hollow tube that protects the entire spinal cord and its nerve roots. The spinal cord runs signals from your brain to the rest of your body and back.
When one or more of these hollow spaces narrows, this is called spinal stenosis. Spinal stenosis can compress your spinal cord and nerve roots. This can cause pain, numbness, weakness, incontinence, and more.
Types of spinal stenosis
There are two main ways doctors categorize spinal stenosis: by general location and by specific narrowing. The 3 general locations are:
- Lumbar (lower back) Spinal Stenosis
- Thoracic (middle back) Spinal Stenosis
- Cervical (upper back or neck) Spinal Stenosis
Lumbar spinal stenosis is the most common and thoracic spinal stenosis is the least common.
The 2 specific narrowings are:
- Foraminal Stenosis: the narrowing of the openings in the spinal column for the exit of the nerve roots.
- Central Canal Stenosis: the narrowing of the main spinal canal.
Foraminal, sometimes called lateral stenosis, is the most common narrowing. It is almost always a result of bone spurs that develop due to arthritis or degenerative disc disease. The narrowing space traps the emerging nerve roots literally pinching the nerves.
Central canal stenosis occurs in any of the vertebrae down the main spinal canal. When the main spinal cord has less space, it can become compressed. This can lead to pain or dysfunction anywhere below the level of compression.
What are the symptoms of spinal stenosis?
Specific symptoms of spinal stenosis determine the location and severity. Symptoms usually develop over time as nerves become more compressed.
However, symptoms can also:
- come and go (be sporadic or have weeks or months of remission);
- occur during certain activities or certain positions;
- be temporarily relieved by rest or flexion (bending forward).
Each general location (lumbar, thoracic, or cervical) has different symptoms. Lumbar stenosis affects the low back, buttocks, and legs. Cervical can also affect the hands, arms, neck, bowel, and bladder more. With thoracic spinal stenosis, you may also feel pain or numbness in your ribs or torso.
The most common symptoms of spinal stenosis include:
- Radicular pain: pain radiating into one arm or one leg (sometimes both). This pain is often described as dull, tender, electric-like, or burning.
- Radiculopathy: numbness, tingling, or weakness in one arm or one leg.
- Myelopathy: numbness, tingling, or weakness in both arms or legs. This can also affect the bladder and/or bowel control.
- Cauda equina syndrome: resulting from the compression of the nerve roots below the spinal cord, it most often displays as saddle numbness and bladder/bowel control issues.
Spinal stenosis usually causes pain. However, in some cases, numbness, weakness, or other symptoms might be present with little or no pain.
What are the causes of spinal stenosis?
The narrowing of the spinal column is often caused by age. As we get older, the tissue in our spine may thicken and compress the nerves.
Some health conditions that can also contribute to stenosis include:
- Ankylosing spondylitis: an inflammatory arthritis affecting the spine and large joints.
- Bulging and herniated discs: a condition where the soft center of a spinal disc pushes through a crack in the disc casing. This can result in pressure on the spinal nerves.
- Degenerative disc disease: the normal wear-and-tear of vertebral discs with age.
- Osteoarthritis: the breakdown of the cartilage in the joints including those in the back can cause stenosis and bone spurs.
- Rheumatoid arthritis: chronic inflammation can cause bone damage and bone spurs to develop in the spine.
- Spinal injury: slipped discs or bone fractures, such as from a car accident, may put pressure on the spinal nerves.
- Tumors: uncommon growths in the spinal canal can trigger inflammation and changes to the surrounding bone.
Other risks and causes include inherited achondroplasia, calcium ossifications (OPPL), Paget’s disease, and scoliosis. You may also be more likely to develop it if it runs in the family or from birth defects.
Treatment for spinal stenosis
In order to diagnose spinal stenosis, BackFit medical professionals will review your medical history and health information, as well as conduct a physical exam. We may also order imaging tests such as x-rays in-house, or an MRI or CT scan if necessary
Treatment for spinal stenosis depends on the results of these tests. Depending on the location and severity, treatment for spinal stenosis often begins with physical therapy. Spinal stenosis is common in people that have become less active. PT can teach you exercises to build your strength and endurance, maintain flexibility and stability, and improve balance.
Other non-surgical treatments that are proven to help include spinal decompression, acupuncture, massage, and gentle chiropractic adjustments. Nutritional advice, including maintaining a healthy weight, may also be provided. Home care remedies can also be helpful including using OTC pain relievers, hot or cold packs, or the use of a cane.
In some cases, we may also prescribe corticosteroid injections to reduce swelling and relieve pain symptoms. If BackFit’s non-invasive treatment plan does not relieve your symptoms, we may refer you to a spinal surgical procedure center as the last option.
More About BackFit
Looking to learn more? Explore our locations, treatments, or our new patient offer below or contact one of the BackFit Family of staff to have your questions answered.